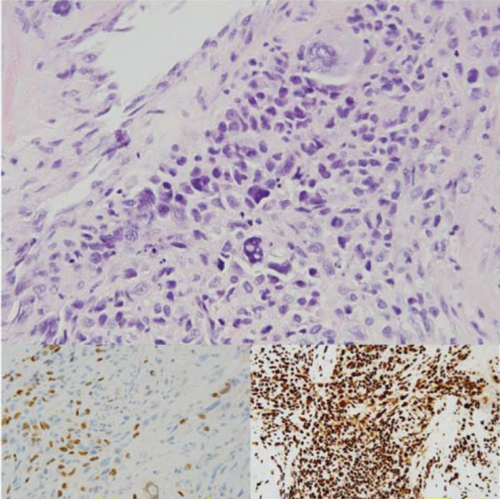
Anaplastic rhabdomyosarcoma in TP53 germline mutation carrier. Image taken from Hettmer et al, Cancer, 2014.
PD Dr. Simone Hettmer
E: simone.hettmer@uniklinik-freiburg.de
T: +49-761-270-45060
Medical Center – University of Freiburg
Center for Pediatrics
Department of Pediatric Hematology and Oncology
Mathildenstraße 1
79106 Freiburg
Germany
Soft-tissue sarcomas are an important challenge in pediatric oncology. These tumors form a heterogeneous group of cancers of non-hematopoietic, mesodermal tissues. They are disproportionately common in children and adolescents. Most patients with high-risk metastatic disease die despite intensive therapy, and those who survive face lifelong, significant late effects of treatment.
Work in the Pediatric Sarcoma Laboratory aims at a better understanding of the cellular, molecular and metabolic underpinnings of sarcomas, which is a prerequisite for improving the diagnostic classification, risk stratification and therapy of these devastating cancers.
TEAM

- Ebrahem Hamed, PhD student
- Eva Jacobs, cand. med.
- Jessica Iftner, cand. med
- Satoshi Nakano, MD
- Micaela Moreno, MD
- Melanie Guimaraes Moreira
- Julia Würtemberger, MD
Alumni
- Sina Angenendt
- Christoph Bauer, PhD student (cooperation with Prof. Dr. Bernd Kammerer, Metabolomics Core Facility, ZBSA Freiburg)
- Meret Quante, cand. med.
- Moritz Petzold, cand. med.
- Michaela Schneider, MTA
- Jakob Siebert, cand. med. (cooperation with Dr. Friedrich Kapp, Department of Pediatric Hematology/ Oncology Freiburg)
- Carla Regina, PhD
- Oliver Uckunkaya
- Mohammad Al-Jumaili
RESEARCH THEMES
Current research in our group includes the following projects:
Plasticity of PAX3:FOXO1 fusion-positive RMS
PAX3:FOXO1 expression in alveolar RMS fluctuates at the single cell level. Our ongoing work aims at demonstrating that PAX3:FOXO1 expression levels correlate with key determinants of malignant behavior and susceptibility to compounds with anti-sarcoma activity.
Asparagine dependence of sarcomas
Sarcoma growth depends on sufficient availability of the non-essential amino acid asparagine. Asparaginase reduces asparagine availability and sarcoma growth. The compensatory mechanisms, utilized by sarcoma cells to counteract the effects of asparagine deprivation, may serve as targets for combination therapies. To modulate asparagine availability in sarcoma cells, we are using lentivirally delivered shRNAs to knock down asparagine synthetase, and we are exposing cells to different concentrations of asparagine. Global metabolomics changes are being evaluated by mass spectrometry to identify actionable adaptive mechanisms. (Moritz Petzold, cand. med.)
Sarcoma predisposition
Recent evidence supports that 12-19% of all sarcomas arise in the context of monogenic, cancer-predisposing germline lesions. We are working on risk assessment tools to identify children with sarcoma-predisposing germline conditions based on full consideration of cancer history, sarcoma manifestation and sarcoma genotype. (Julia Würtemberger, MD & Manching Ku, PhD)
TP53 in RMS
We are investigating the impact of aberrant TP53, introduced at different time points during tumor evolution, on rhabdomyosarcoma phenotype, target expression and treatment susceptibility. (Ebrahem Hamed, PhD student)
For information about our pediatric sarcoma/sarcoma predisposition clinic, please visit the Sarcoma Clinic pages on the website of the Freiburg Center for Pediatrics and Adolescent Medicine.
SELECTED RECENT PUBLICATIONS
Complete list of published works by Simone Hettmer: https://www.ncbi.nlm.nih.gov/myncbi/101blyh9NiOAL/bibliography/public/
-
Lack of Electron Acceptors Contributes to Redox Stress and Growth Arrest in Asparagine-Starved Sarcoma Cells. Cancers (Basel). Bauer C, Quante M, Breunis WB, Regina C, Schneider M, Andrieux G, Gorka O, Groß O, Boerries M, Kammerer B, Hettmer S. 2021 Jan 22;13(3):412. doi: 10.3390/cancers13030412. PMID: 33499165; PMCID: PMC7865502.
-
Negative correlation of single-cell PAX3:FOXO1 expression with tumorigenicity in rhabdomyosarcoma. Regina C, Hamed E, Andrieux G, Angenendt S, Schneider M, Ku M, Follo M, Wachtel M, Ke E, Kikuchi K, Henssen AG, Schäfer BW, Boerries M, Wagers AJ, Keller C, Hettmer S.Life Sci Alliance. 2021 Jun 29;4(9):e202001002. doi: 10.26508/lsa.202001002. PMID: 34187933; PMCID: PMC8321661.
-
Combinatorial effects of azacitidine and trametinib on NRAS-mutated melanoma. Hanft KM, Hamed E, Kaiser M, Würtemberger J, Schneider M, Pietsch T, Feige U, Meiss F, Krengel S, Niemeyer C, Hettmer S. Pediatr Blood Cancer. 2022 Apr;69(4):e29468. doi: 10.1002/pbc.29468. Epub 2021 Dec 6. PMID: 34866327.
-
Genetic susceptibility in children, adolescents, and young adults diagnosed with soft-tissue sarcomas. Würtemberger J, Ripperger T, Vokuhl C, Bauer S, Teichert-von Lüttichau I, Wardelmann E, Niemeyer CM, Kratz CP, Schlegelberger B, Hettmer S. Eur J Med Genet. 2023 May;66(5):104718. doi: 10.1016/j.ejmg.2023.104718. Epub 2023 Feb 9. PMID: 36764384.
- Patterns of Prior and Subsequent Neoplasms in Children and Adolescents With Soft Tissue Sarcomas. Uckunkaya O, Nöllke P, Hallmen E, Becker C, Stegmaier S, Sparber-Sauer M, Vokuhl C, Koscielniak E, Hettmer S. J Pediatr Hematol Oncol. 2020 Jul;42(5):e265-e270. doi:10.1097/MPH.0000000000001837
- Analysis of the relationship between the KRAS G12V oncogene and the Hippo effector YAP1 in embryonal rhabdomyosarcoma. Mohamed AD, Shah N, Hettmer S, Vargesson N, Wackerhage H. Sci Rep. 2018;8(1):15674. Published 2018 Oct 23. doi:10.1038/s41598-018-33852-7
- Anaplastic rhabdomyosarcoma in TP53 germline mutation carriers. S Hettmer*, NM Archer, GR Somers, A Novokmet, AJ Wagers, L Diller, C Rodriguez-Galindo, LA Teot, D Malkin. Cancer. 2014 Apr 1;120(7):1068-75 (* corresponding author). doi:10.1002/cncr.28507.
- Cell-cycle dependent expression of a translocation-mediated fusion oncogene mediates checkpoint adaptation in rhabdomyosarcoma. K Kikuchi, S Hettmer, MI Aslam, JE Michalek, W Laub, BP Rubin, AJ Wagers, C Keller. PLOS Genetics. 2014;10(1):e1004107. doi:10.1371/journal.pgen.1004107
- Isolation of progenitors that exhibit myogenic/osteogenic bipotency in vitro by fluorescence activated cell sorting from human fetal muscle. A Castiglioni* and S Hettmer*, MD Lynes, TN Rao, D Tchessaolova, I Sinha, BT Lee, YH Tseng, AJ Wagers. Stem Cell Reports. 2014;2(1):92-106 (* shared first authorship). doi:10.1016/j.stemcr.2013.12.006
- The Hippo Transducer YAP1 Transforms Activated Satellite Cells and is a Potent Effector of Embryonal Rhabdomyosarcoma Formation. AM Tremblay, E Missiaglia, GG Galli, S Hettmer, R Urcia, M Carrara, RN Judson, K Thway, G Nadal, JL Selfe, G Murray, RA Calogero, C De Bari, PS Zammit, M Delorenzi, AJ Wagers, J Shipley, H Wackerhage and FD Camargo. Cancer Cell. 2014 Aug 11;26(2):273-87. doi:10.1016/j.ccr.2014.05.029
- Functional genomic screening reveals asparagine dependence as a metabolic vulnerability in sarcoma. S Hettmer, AC Schinzel, D Tchessalova, M Schneider, CL Parker, R Bronson, NG Richards, W Hahn, AJ Wagers. Elife. 2015 Oct 24;4. doi:10.7554/eLife.09436
- Clinical and mutational spectrum of highly differentiated, PAX:FOXO1 fusion-negative rhabdomyosarcoma. L Teot, M Schneider, AR Thorner, J Tian, Y Chin, M Ducar, L Lin, M Wlodarski, HE Grier, CMD Fletcher, P van Hummelen, SX Skapek, DS Hawkins, AJ Wagers, C Rodriguez-Galindo, S Hettmer. Cancer. 2018 Feb 20. doi:10.1002/cncr.31286
COLLABORATIONS, CO-OPERATIONS AND NETWORKS
- Prof. Dr. Beat Schäfer, KISPI, Experimentelle Infektiologie und Krebsforschung, Universität Zürich
- Prof. Dr. Dr. Melanie Börries, Institute of Medical Bioinformatics and Systems Medicine, Medical Center-University of Freiburg
- Prof. Dr. Olaf Groß, Institute of Neuropathology, Medical Center, University of Freiburg
- Dr. Oliver Schilling, University of Freiburg
- PD Dr. David Braig, University of Freiburg
- PD Dr. Peter Bronsert, University of Freiburg
- Dr. Katalin Komlosi, University of Freiburg
- PD Dr. Irene von Lüttichau, München
- INSTRuCT, Epicycle Konsortium